![]()
Diary March 2002
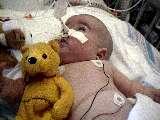
Mar 3 2002 News: After momentarily improving, Saffy's respiratory problems worsened, and she was put back on the BiPAP yesterday. Unfortunately, her condition continued to degrade, and she was reintubated early this morning and transferred back to the main PICU. Her doctors suspect a respiratory infection; but, so far, all tests have returned negative. We will post more details soon.
 |
|
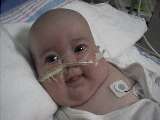
Saffy before reintubation |
Mar 4 2002 News: We were hoping Saffy would be home soon; but, unfortunately, she took a slide backward. For the week and a half she was off the ventilator, she was breathing very fast and was spitting up a lot. Last week, she was able to recover from the partial collapse of her right lung, but the problem recurred in both lungs. Saffy was unable to recover this time and was reintubated early Sunday morning.
Saffy’s doctors were not sure why her breathing was labored but believe her latest respiratory problems are due to a cold. All the tests for common viruses and infections have been negative, but they can’t test for everything. Interestingly, Alec got a cold at the same time. Saffy’s immune system is compromised due to the anti-rejection medications she requires to keep her transplanted liver, so she is more susceptible to viruses and infections and has a harder time recovering.
Saffy will now need to build up her strength--hopefully weaning her from the vent won’t be as difficult this time. In the meantime, Saffy is scheduled for another CT scan tomorrow to detect any evidence of tumor recurrence.
Saffy’s thyroid levels have been normal, but her endocrinologists want to keep her on Synthroid. Originally, they mentioned stopping the medication, but they now want to leave her on it for her first three years, which is the most important growth period for the brain. As long as she doesn’t go into hyperthyroidism, the dose will remain the same.
Saffy's doctors aren’t too concerned that she has not grown much in the last few months. It's to be expected with the traumatic situation she has been through. The calories she is receiving have again been increased, and they now expect her to resume growing.
In other news, we're pleased to announce that Saffy will soon be a big sister. Jill is expecting again; and, based on a preliminary ultrasound, her due date is August 23. Coincidently, that will be Saffy's first birthday.
We learned the good news in January when Jill was being tested to be a live liver donor for Saffy. The pregnancy is the reason Jill wasn’t a suitable donor. We're overjoyed to expand our family; but, at the time we learned the news, we were worried that we would lose Saffy. Luckily, Saffy received a liver from a cadaveric donor soon afterwards. Many children have to wait months or years for a liver transplant, but Saffy's extreme condition put her on the top of the list.
Organ donation saved our daughter's life. Please support organ donation and discuss your wishes to donate with your family. Signing an organ donor card is important, but hospitals require your family's permission before donation. Make sure your family members understand your wishes.
Mar 5 2002 News: We have some unfortunate news. Saffy's best friend and companion was also diagnosed with hepatic infantile hemangioendothelioma and angiosarcoma. Luckily, a donor was quickly located, and Poopsie underwent an emergency liver transplant today. The surgery took 11 minutes, and he is now recovering nicely.
 |
|
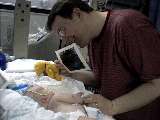
Daddy shows Saffy an ultrasound picture of her younger brother or sister |
Mar 7 2002 News: Our doctors heard back from AFIP, and their pathologists confirmed that Saffy's excised liver contained angiosarcoma. AFIP's 2001 publication on liver tumors also cleared up our misunderstanding of the terms used. Previous medical texts differentiated between infantile hemangioendothelioma type 2 and angiosarcoma (and identified the former as benign and the latter as malignant), but they "now consider [the] 'type 2' lesion an angiosarcoma" called pediatric angiosarcoma. Further, due to some features different from angiosarcoma in adults, they propose calling it kaposiform angiosarcoma.
AFIP's book states, "Most children with angiosarcoma of the liver have died within 2 years; the mean survival period in [a study] was 10 months. Therapy, consisting of surgery, radiotherapy, chemotherapy, or combinations thereof, has been ineffective." Saffy remains unimpressed. She's a tough little girl, and we have high hopes that she will beat this disease.
We continue to discuss treatment possibilities with Saffy's doctors. They have generally not wanted to use chemotherapy due to the very high risks involved. At this point, if she were to receive the chemo doses necessary to combat angiosarcoma, she probably wouldn't survive. However, her doctors were considering chemo after a couple more months of growth and recovery. Even then, the chemo would be very dangerous; but, if the angiosarcoma has such a high probability of recurrence, the risks may be worth it.
The decision whether to use chemo would be based on the probability of the angiosarcoma returning. For example, if it recurs in 80% of cases, the chemo would probably be worth the risk. Unfortunately, with so few reported cases of pediatric angiosarcoma, it's impossible to predict. We have found reports of three children (and 14 adults) who received liver transplants for angiosarcoma, and none of them survived; but, once again, that's not enough cases in which to base a prediction. Due to this uncertainty, Saffy's doctors are currently recommending chemo not be administered.
Saffy's doctors previously discussed performing a biopsy of her cutaneous (skin) hemangiomas due to fears that they also could be malignant, but all her doctors are now in agreement that they are benign and a biopsy is unnecessary.
The good news is that Saffy underwent another full body CT scan the day before yesterday, and there is no evidence of tumors in her new liver or other organs. Hopefully, it won't return. Saffy will probably undergo CT scans every 2-3 months for the foreseeable future.
Saffy is still on the ventilator. Her doctors are still uncertain why she continues to have respiratory difficulties. Some thought her latest problems were due to a virus, but that's probably not true (since all the tests were negative, and she's no longer showing symptoms--which would be an amazingly quick recovery for an infant on immunosuppressants). A virus is yet another theory (along with diaphragm damage and hemangiomas in her airway) that has been eliminated. The latest theory is that she is silently aspirating small amounts of formula into her lungs. Her feeding tube is now being passed further down--past her stomach and into her small intestines--to eliminate the possibility of formula getting into her lungs. She is still spitting up a lot of mucous though.
Her doctors are going to delay weaning her off the vent for a few days, so she can rest and hopefully grow. In addition to high calorie formula, she is also receiving lipids (fat) and a supplement which is much like an energy bar. They will probably try to extubate next week.
And, oh yes, Poopsie's recovery from his liver transplant is going well. He says the immunosuppressants "taste funky."
 |
|
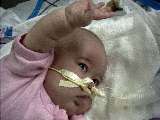
Saffy waves to her fans |
Mar 12 2002 News: Saffy has improved and gained a little weight. She is being weaned from the ventilator again, and the plan was to attempt extubation tomorrow. Unfortunately, that has been delayed, because her doctors believe that the last CT scan shows a piece of the Broviac--that was removed in January--still lodged in her femoral vein. However, it may just be an artifact of the image, so she is scheduled for yet another CT scan tomorrow to confirm. If it is the Broviac, they will see if it has traveled and how they can remove it. She may need to undergo surgery.
Otherwise, Saffy has done relatively well. Her LFTs are still good, and her steroid dose was reduced. She continues to spit up a lot of mucous, and her doctors suspected that this might be a sign of cystic fibrosis, but a sweat test came back negative. Her hair is beginning to regrow, so she now looks like a skinhead.
Mar 13 2002 News: Saffy underwent another CT scan today, and it turns out the suspected Broviac piece was a wild goose chase. It was an image artifact of the last scan--probably a line of contrast (IV dye used to improve visibility) passing through her vein.
This was Saffy's tenth CT scan and further scans are planned for every 2-3 months. She has also undergone scores of x-rays and a fluoroscopy. The amount of radiation she has received--and the associated increased risk of developing cancer--is a concern, but the benefits certainly outweigh the risks. Just another thing for which her parents can worry!
After the CT scan, Saffy was extubated late today. She appeared to do well off the ventilator, so her doctors skipped the BiPAP. She is breathing on her own with the assistance of supplemental oxygen. Saffy's prior extubation attempts lasted an hour, nearly a day, and nearly two weeks. Hopefully this fourth attempt will last the rest of her long, fruitful life.
 |
|
Jill, Saffy, and the new baby (behind Saffy) |
Mar 15 2002 News: Saffy is doing well off the ventilator. So far so good. She even went without supplemental oxygen for a short time this afternoon. She's a bit restless--which is probably just due to withdrawal from sedation--but she has been in a good mood with lots of smiles.
We would like to thank The Brittany Miller Foundation for their support. Brittany Miller was a young girl who died on her seventh birthday after fighting a spirited battle against brain cancer. The Foundation helps families who have children undergoing cancer treatment with incidental expenses such as travel and lodging costs.
Mar 18 2002 News: Saffy continues to do well off the ventilator. She still requires supplemental oxygen, but her doctors think she may be able to come home soon. Physical therapy has resumed, and she is making progress.
Mount Sinai is in the news [link updated] again about problems with the adult liver transplant program, but we have nothing but good things to say about the care Saffy is receiving.
Mar 22 2002 News: Saffy was doing so well off the ventilator; but, unfortunately, she took a turn for the worse. She began having breathing difficulties on Tuesday and then declined rather rapidly. She was reintubated on Wednesday. Her doctors are puzzled why she is still having trouble breathing on her own, and they are exploring a number of theories. More details to follow.
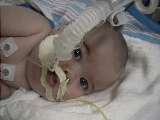 |
|
Saffy back on the vent |
Mar 23 2002 News: Saffy is 7 months old today. She is still on the ventilator while her doctors discuss next steps. They're really not certain what is causing her breathing difficulties. Past theories that were ruled out included diaphragm damage, hemangiomas in her airway, and a virus. The latest theory was that she was aspirating small amounts of formula into her lungs. She seemed to have more trouble when she had an NG tube, which goes through a nostril into her stomach--where reflux is possible--and showed improvement with an ND tube, which goes past her stomach into her duodenum (the first part of the small intestine)--which pretty much eliminates the possibility of reflux and/or aspiration. However, her doctors are still not certain that explains her breathing problems. They had planned a nuclear milk study to see if formula could be detected in her lungs, but the study is not possible while intubated.
Saffy's doctors again suspected a problem with her airway--either hemangiomas, scarring from being intubated, or an anatomical blockage. A scope was used at bed-side, and they didn't see any problems, but they could only see down to her vocal chords. They are again discussing a bronchoscopy--which is performed in the operating room--so they can see her entire airway down to her lungs. Of course, a bronchoscopy is a somewhat invasive procedure, and it could cause further irritation--perhaps even requiring a tracheostomy.
The NG/ND tube could be causing irritation as well. Even if Saffy's airway is not restricted and the problem is aspiration, an ND tube is not a long-term solution, because it must be managed in the hospital (unlike an NG tube which can be managed at home). Either way, it is beginning to look like an enterostomy--where a tube is surgically inserted through the abdomen into the stomach (gastrostomy) or intestine (jejunostomy)--may be needed. Either one would bypass the airway, but a j-tube is probably preferred over a g-tube because, much like ND and NG tubes, bypassing the stomach eliminates reflux.
Obviously, feeding and breathing is a complicated subject--especially in a critically ill infant--and many different possible causes and solutions are being discussed. Saffy's doctors cover a wide range of pediatric specialties, and they are now working to come to a consensus and a plan of action. Our preference is to avoid a trach and get her off the vent--perhaps a j-tube can accomplish that.
Besides that big issue, Saffy is doing well liver-wise and has put on more weight. Her hair is growing back; but, unfortunately, a couple spots were shaved during several unsuccessful attempts to place an IV. Eventually, they had to put a central line in her thigh. She will also need another blood transfusion soon. Finally, her endocrinologists suspected she may have hypercalcemia, but an EKG ruled it out.
Mar 25 2002 News: The current plan is for Saffy to undergo a bronchoscopy later this week. The next steps will depend on the results; but, hopefully no problems will be discovered and extubation can be attempted again.
Mar 28 2002 News: Saffy underwent a laryngoscopy/bronchoscopy in the operating room this morning. The biggest concern was that she had hemangiomas or scarring in her airway that would require a tracheostomy. Luckily, no such major problems were found. However, they did discover granulation (unwanted tissue growth) and swelling around her vocal cords caused by irritation from the endotracheal (ET) tube, which is connected to the ventilator and passes down her mouth or nose to her airway. Below her larynx is clear, and the surgeons didn't see any evidence of her heart pressing against her airway.
The swelling around her vocal cords makes it harder for her to breathe. It significantly constricts her airway. The inflammation will need to be reduced in order for her to breathe without assistance; however, the irritation will continue as long as the ET tube is in place. It's a bit of a catch-22: the ET tube needs to be removed in order to reduce the swelling, but it's needed for her breathe as long as there is swelling.
Saffy's doctors want to give her one more chance at extubation. The steroids she receives as an immunosuppressant for her liver transplant were recently reduced, but now they have switched her to a different kind and increased the dosage (via IV instead of oral) in order to reduce the inflammation around her vocal cords. She is also getting increased sedation, so she won't move around as much and cause the ET tube to rub against her larynx. After a couple days, giving the steroids time to work, her doctors will extubate again.
If Saffy is unable to breathe without the ventilator, her doctors say she will need a tracheostomy. It will bypass her vocal cords and the interference with feeding and give her a chance to grow and get stronger. However, a trach could mean Saffy will be on a ventilator for--if not months--years. Researching other children at such sites as www.tracheostomy.com shows that usually the trach isn't removed until the child is three to five years of age.
Our hope, of course, is that Saffy succeeds in breathing without assistance and a tracheostomy is unnecessary.
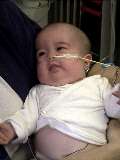 |
|
Saffy after extubation #5 |
Mar 30 2002 News: For the past two days, Saffy has received increased doses of steroids to shrink her swollen vocal cords and additional sedation so her movements won't cause more irritation from the ET tube. All sedation and feeds were halted this morning, and she was extubated. So far, she is breathing fine with only a small amount of supplemental oxygen. However, she has been grumpy due to the trauma of extubation plus the reduction (and associated withdrawal) of sedation. She was restarted on small amounts of sedation later in the afternoon and is also receiving methadone to help with withdrawal. Her feeding tube was passed further down (now an ND tube), so feeding was later resumed. Hopefully the fifth time's the charm!
![]() www.usticke.org
Saffy Liver Condition Home
www.usticke.org
Saffy Liver Condition Home
![]() Previous
Saffy Liver Condition Diary - Next Saffy Liver Condition Diary
Previous
Saffy Liver Condition Diary - Next Saffy Liver Condition Diary![]()